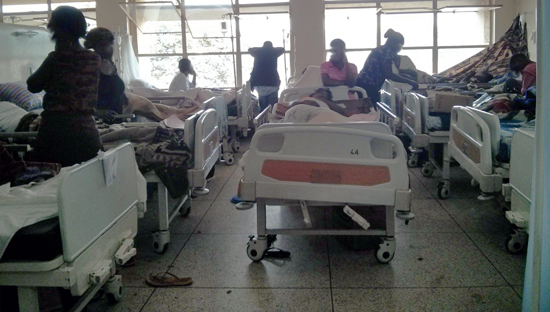
Bilal Jawed ’17 – Welcome to Ward 4C in Mulago Hospital, the last stop for many HIV patients and my second home for this summer. Understandably, one of the most common questions I get asked by senior members of the team is: “[H]ow are you getting used to the ward?”
It is very difficult for me to capture the atmosphere of the Ward: the sights, the sounds, and the smells. You can practically feel the sickness in the air and touch it. Perhaps it is best to begin with the familiar.
Imagine your last hospital stay, and if you are fortunate enough to never have been admitted into a hospital, think back to visiting a friend or loved one. Maybe you are dropping by to sign a cast, welcome a little one into the family, or give your well wishes after a successful surgery. You probably have a room to yourself, a nurse that visits every hour or so, clean bedding, and food to ensure the best chance at recovery. When you go to bed, you feel comforted by the fact that the best doctors armed with nearly unlimited medications and technology will be present if anything were to go wrong.
Now, welcome to 4C. First remove your individual room and replace it with a large, open-aired room, packed to the brim with hospital beds. Inches to your left, right, and at your feet, are beds of literally the sickest people in the world. People battling HIV along with tuberculosis, meningitis, malaria, hepatitis, rabies, or most often, a combination of several infectious diseases. When you go to bed at night, you can hear your neighbor convulsing from a seizure, or someone across the room moaning from pain. In the morning, you can smell people who urinated or defecated on themselves, or hear the cries of a family mourning someone who did not make it though the night. You depend on your family to visit you, clean your sheets and feed you, because the hospital does not have the proper resources or staff to provide them for you. At the same time, you are fighting your own battle. Not a broken arm or the flu, but diseases that require the best care in the world — but sadly, you do not have the best care in the world because you belong to Ward 4C.
Now that we’ve seen a glimpse of the patient’s perspective, I’d like to quickly and briefly shift to the doctor’s challenges (a topic to be revisited in a future blog). From Day 1 when the patient is admitted, it is a race to get him or her discharged. Especially because we deal with HIV patients with already weakened immune systems, hospital acquired infections (HAIs) are a real danger. This took me a long time to grasp—the ward, where people go to heal, can actually be a source of illness because of the high concentration of already very sick people. Moreover, with limited availability of drugs and equipment like ventilators and MRI machines, it is like fighting a goliath blindfolded. The challenge ahead is already so monstrous, but handicaps we face make it just that much harder. In fighting the “Goliaths”, there is definitely a danger to the “Davids”—stress, emotional struggles, or even worse. While many of the doctors and nurses that I have spoken to won’t admit it, there is certainly a health risk of just working in Ward 4C. TB is in the air, and HIV+ infected needles are everywhere. I myself have handled HIV+ needles and cerebrospinal fluid containing HIV (of course, having received the proper training and precautions). While these are trained professionals and historical occupational exposure is relatively low, it is always frightening knowing that you are a single accident away from needing post-exposure prophylaxis.
The week before my flight to Uganda, I was hit with the news that my father had a heart attack. Instead of taking my Chemistry final, I was spending nights in the hospital back in Indianapolis with my father awaiting and following his open-heart surgery. While we were all nervous, I knew in the back of my head that everything would be fine because at the end of the day, I trusted the quality of care. Fast forward only a week and half and I can’t say the same for the patients battling HIV/meningitis. I’m glad to be witnessing these harsh realities firsthand. For both the patients and the doctors, it truly is a war out here, but I am glad to be apart of it in anyway I can.
More to come about working on a clinical drug trial in Kampala!